Evidence has shown that vestibular rehabilitation can be effective in improving symptoms related to many vestibular – inner ear – disorders.1, 2 People with vestibular disorders often experience problems with vertigo, dizziness, visual disturbance, and/or imbalance. These are the problems that rehabilitation aims to address. Other problems can also arise that are secondary to the vestibular disorder like nausea and/or vomiting, reduced ability to focus or concentrate, and fatigue.
Symptoms due to vestibular disorders can diminish quality of life and can impact all aspects of life from economic to social participation as well as can contribute to emotional problems, like anxiety and depression. Additionally, one of the consequences of having a vestibular disorder is that the symptoms frequently cause people to adopt a sedentary lifestyle in order to avoid bringing on, or worsening, dizziness and imbalance that occurs with movement. As a result, decreased muscle strength and flexibility, increased joint stiffness, and reduced stamina can occur from this lifestyle. Treatment strategies used in rehabilitation can also be beneficial for these secondary problems.
What is vestibular rehabilitation?
Vestibular rehabilitation (VR) is a specialized form of therapy intended to alleviate both the primary and secondary problems due to vestibular disorders. It is an exercise-based program primarily designed to reduce vertigo and dizziness, reduce gaze instability, and/or reduce imbalance and fall risk as well as address any secondary impairments that are a consequence of the vestibular disorder.
For most people who have a vestibular disorder, the deficit is permanent because the amount of restoration of vestibular function is very small. However, after vestibular system damage, symptoms can reduce and function can improve because of compensation. This occurs because the brain learns to use other senses (vision and somatosensory – body sense) to substitute for the deficient vestibular system. For many, compensation occurs naturally over time, but for patients whose symptoms do not reduce and who continue to have difficulty returning to daily activities, VR can assist in recovery by promoting compensation.3
The goal of VR is to use a problem-oriented approach to promote compensation. This is achieved by customizing exercises to address the specific problem(s) of each individual. Therefore, before an exercise program can be designed, a comprehensive clinical examination is needed to identify problems related to the vestibular disorder. Depending on the vestibular-related problem(s) identified, three principal methods of exercise can be prescribed: 1) Habituation, 2) Gaze Stabilization, and/or 3) Balance Training.4
Habituation exercise
Habituation exercise is used to treat symptoms of dizziness that is produced because of self-motion3 and/or produced because of visual stimuli.5, 6 Habituation exercise is indicated for patients who report increased dizziness when they move around, especially when they make quick head movements, or when they change positions like when they bend over or look up to reach above their heads. Also, habituation exercise is appropriate for patients who report increased dizziness in visually stimulating environments, like shopping malls and grocery stores, when watching action movies or T.V., and/or when walking over patterned carpets and shiny floors. The goal of habituation exercise is to reduce the dizziness through repeated exposure to specific movements or visual stimuli that provokes patients’ dizziness. These exercises are designed to mildly, or at the most, moderately provoke the patients’ symptoms of dizziness. Over time, with good compliance and perseverance, the dizziness intensity can reduce due to the brain learning to ignore the abnormal signal.
Gaze Stabilization
Gaze Stabilization exercises are used to improve control of eye movements so vision can be clear during head movement. These exercises are appropriate for patients who report problems seeing clearly because their visual world appears to bounce or jump around, such as when reading or when trying to identify objects in the environment, especially when moving about. There are two types of eye and head exercises used to promote gaze stability. The choice of which exercise(s) to use depends on the type of vestibular disorder and extent of the disorder.
One example is:
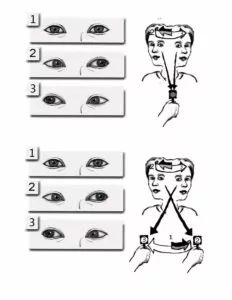
Image by Karen Ilari, © VeDA
Balance Training exercises
Balance Training exercises are used to improve steadiness so that daily activities for self-care, work, and leisure can be performed successfully. Exercises used to improve balance should be designed to address each patient’s specific underlying balance problem(s).7 Also, to promote changes in balance, the exercises need to be moderately challenging, but safe enough so patients do not fall while doing them.
Additionally, balance exercises should be designed to reduce environmental barriers and fall risk. For example, the exercises should help improve patients’ ability to walk outside on uneven ground or walk in the dark.
For patients with Benign Paroxysmal Positional Vertigo (BPPV), the exercise methods described above are not appropriate to resolve this type of vestibular disorder. Through assessment, the type of BPPV is identified, and depending on the type, different repositioning maneuvers can be performed to help resolve the spinning that occurs due to position changes.8, 9
What Should Patients Expect From Vestibular Rehabilitation?
VRT is usually performed on an outpatient basis, although in some cases, the treatment can be initiated in the hospital. Patients are seen by a licensed physical or occupational therapist with advanced post-graduate training.
VRT begins with a comprehensive clinical assessment that should include collecting a detailed history of the patient’s symptoms and how these symptoms affect their daily activities. The therapist will document the type and intensity of symptoms and discuss the precipitating circumstances.
Additionally, information about medications, hearing or vision problems, other medical issues, history of falls, previous and current activity level, and the patient’s living situation will be gathered.
The assessment also includes administering different tests to more objectively evaluate the patient’s problems. The therapist will screen the visual and vestibular systems to observe how well eye movements are being controlled. Testing assesses sensation (which includes gathering information about pain), muscle strength, extremity and spine range of motion, coordination, posture, balance, and walking ability.
A customized exercise plan is developed from the findings of the clinical assessment, results from laboratory testing and imaging studies, and input from patients about their goals for rehabilitation. For example, a person with BPPV may undergo a canal repositioning exercise for the spinning s/he experiences, whereas, someone with gaze instability and dizziness due to vestibular neuritis (a deficit from a weakened inner ear) may be prescribed gaze stability and habituation exercises, and if the dizziness affects their balance this may also include balance exercises.
An important part of the VRT is to establish an exercise program that can be performed regularly at home. Compliance with the home exercise program is essential to help achieve rehabilitation and patient goals.
Along with exercise, patient and caregiver education is an integral part of VRT. Many patients find it useful to understand the science behind their vestibular problems, as well as how it relates to the difficulties they may have with functioning in everyday life. A therapist can also provide information about how to deal with these difficulties and discuss what can be expected from VRT. Education is important for patients because it takes away much of the mystery of what they are experiencing, which can help reduce anxiety that may occur as a result of their vestibular disorder.
Are Vestibular Rehabilitation Exercises Difficult To Do?
The exercises are not difficult to learn, but that doesn’t mean they are easy to do!
The exercises can sometimes be tedious; however, committing to doing them is key to helping you achieve success. Setting up a regular schedule so that you incorporate them into your day is very important.
Exercises may, at first, make your symptoms seem worse. But with time and consistent work, your symptoms should steadily improve, and then, you will find that you are able to participate more in the activities of your daily life.
Factors That Can Impact Recovery
When patients participate in VR, different factors can impact the potential for recovery. For example, the type of vestibular disorder affects recovery. Patients that have a stable vestibular disorder, such as vestibular neuritis or labyrinthitis, have the best opportunity to have a satisfactory resolution of symptoms. When patients have a progressive vestibular disorder, like with multiple sclerosis, or a fluctuating condition, like with Migraine and Meniere’s, which causes spontaneous attacks of dizziness or vertigo, compensation can be difficult to achieve, and therefore, success with VR is more difficult. There are also differences in response to VR depending on whether you have one or both inner ears involved, or whether the problem lies within the vestibular parts of the brain as opposed to the ear(s).
Other factors that can potentially limit recovery:
Symptomatic relapses can occasionally occur because the brain de-compensates. This can be due to different emotional and/or physical stressors, like personal or job-related pressures, periods of inactivity, a bad cold or flu, extreme fatigue or chronic lack of sleep, changes in medication, or sometimes surgery.3 Although it is important for patients to consult with their physician to make sure nothing new has occurred, returning to the exercises that promoted the initial compensation can help promote recovery again. Additionally, recovery after de-compensation usually occurs more quickly as compared to the initial compensation.
Where can I find a vestibular rehabilitation specialist?
The Vestibular Disorders Association (VeDA) provides a directory of health professionals who are specially trained to assess and treat vestibular disorders. This online directory offers users the ability to search for providers according to specialty and geographical location. To locate this online directory, visit vestibular.org/healthcare-directory.
Author: Lisa Farrell, PT, PhD, AT,C; Clinical Faculty, Department of Physical Therapy, Nova Southeastern University, Fort Lauderdale, FL

 REGain Your Mobility with Activator Poles
REGain Your Mobility with Activator Poles